Integrated Therapy for Bipolar Disorder – A Holistic Approach
If you or someone you love lives with bipolar disorder, you already know the hardest part is not “having mood swings.” It’s the unpredictability. The way a good week can turn into a sleepless, wired stretch of overconfidence. Or how a low mood can quietly thicken into a depression that feels physically heavy.
Bipolar disorder is also far more common than most people realize. The World Health Organization estimates about 1 in 200 people worldwide live with bipolar disorder. And the impact is serious, bipolar disorder is associated with disability, relationship strain, work disruption, and a higher risk of self-harm and suicide.
So what actually helps in real life, beyond generic advice?
At Mind Brain Institute, we lean on a simple principle: integrated therapy for bipolar disorder. Not because one approach is “wrong,” but because bipolar disorder sits at the intersection of biology, psychology, and lifestyle rhythms. The most reliable outcomes often come from psychiatry + psychotherapy + (when needed) neuromodulation, delivered as a coordinated plan rather than three disconnected services.
That’s what this blog is about: how integrated care works, who it’s for, and why it can change the trajectory of recovery.
What Is Integrated Therapy for Bipolar Disorder
Integrated therapy for bipolar disorder means your treatment is designed as one connected system. Instead of treating medication, therapy, and advanced interventions as separate “add-ons,” integrated care combines them into a single plan with shared goals, consistent monitoring, and clear communication. In practical terms, this usually includes:
- Psychiatry to stabilize mood biology (and to keep medication safe and effective over time)
- Psychotherapy to strengthen insight, reduce relapse triggers, and build coping tools that last
- Neuromodulation when symptoms, especially depression – do not respond enough to standard treatment
This approach also supports something many people underestimate: bipolar disorder is often a long-term condition, but it does not have to be a life sentence of chaos. The goal is not “perfect moods.” The goal is stable functioning, fewer relapses, faster recovery when episodes happen, and better quality of life.
Why Does Bipolar Disorder Require an Integrated Approach
Bipolar disorder is not only about mood. It affects:
- sleep and circadian rhythm
- impulse control and decision-making
- energy regulation
- thinking speed and focus
- relationships and work performance
That’s why a single-track solution can fail. For example, medication may reduce intensity, but without therapy and routine-building, triggers keep repeating. Therapy may help emotionally, but without mood stabilization, the brain may stay vulnerable to episodes.
And the stakes are real. Research reviews consistently show elevated suicide risk in bipolar disorder, including substantial lifetime rates of suicide attempts and deaths compared with the general population. This is exactly why “trial and error” care without consistent follow-up can be dangerous.
Integrated therapy for bipolar disorder reduces gaps. It creates a safety net where relapse signs are spotted early, adjustments happen faster, and the person is treated as a whole human, not a diagnosis.
How Does Psychiatry Support Mood Stabilization
Psychiatry forms the biological foundation of care. Bipolar disorder has a strong neurochemical component, and mood stabilizing medications often play a critical role in reducing the intensity and frequency of episodes.
However, effective psychiatric care is not simply about prescribing medication. It involves careful diagnosis, selecting the appropriate mood stabilizer, monitoring side effects, and regularly reviewing symptom patterns. Many people experience partial responses at first. Fine tuning is part of the process.
At Mind Brain Institute, psychiatric care focuses on long term stability. We closely monitor sleep patterns, stress levels, and subtle behavioral shifts that may signal an upcoming episode. Medication becomes one part of a larger, continuously evaluated plan.
How Does Psychotherapy Improve Long Term Stability
While psychiatry stabilizes mood biology, psychotherapy strengthens emotional regulation and insight.
Therapy for bipolar disorder often focuses on identifying early relapse triggers, improving adherence to treatment, and building structured daily rhythms. Psychoeducation is especially powerful. When you understand how your mood cycles behave, you gain the ability to intervene earlier.
Cognitive behavioral therapy helps challenge depressive thought patterns and encourages protective behaviors during vulnerable phases. Family focused therapy can reduce conflict and create a supportive environment that recognizes early warning signs rather than reacting to full blown episodes.
Therapy turns knowledge into skill. It gives you tools that remain useful even during stable periods.
What Role Does Neuromodulation Play in Integrated Therapy for Bipolar Disorder
Here’s the part many people do not hear about until they have been struggling for a long time.
Sometimes, bipolar depression does not respond enough, even with good medication and therapy. This can feel especially defeating because depression in bipolar disorder can be more frequent and longer-lasting than manic episodes for many individuals.
In those cases, neuromodulation becomes a meaningful option. One of the most widely discussed and studied methods today is Transcranial Magnetic Stimulation (TMS), a non-invasive treatment that uses magnetic pulses to influence brain circuits involved in mood regulation.
Recent reviews and analyses suggest rTMS can be effective for bipolar depression, with ongoing research into which protocols and patient profiles respond best.
Important: neuromodulation is not a “replacement” for integrated care. It works best when it’s part of a coordinated plan, because mood stability still depends on follow-up, routine protection, and long-term relapse prevention.
At Mind Brain Institute, this is how we think about it:
- Psychiatry sets stability and safety
- Therapy builds resilience and relapse prevention
- Neuromodulation can help “unstick” difficult depressive circuitry when standard options are not enough
When Is Integrated Therapy for Bipolar Disorder Most Beneficial
Integrated care is helpful for many people, but it becomes especially important if you recognize any of these:
- repeated relapses or frequent mood cycling
- persistent bipolar depression despite treatment
- hospitalization history or high-risk periods
- severe functional impact at work or home
- medication side effects causing poor adherence
- family stress, conflict, or lack of support
- co-occurring anxiety, substance use, or trauma symptoms
If you’ve ever felt like you’re “collecting treatments” without a clear strategy – one doctor here, one therapist there, a new medication every few months, integrated therapy for bipolar disorder can be the shift from patchwork to plan.
How Does a Holistic Approach Strengthen Recovery
This is where “holistic” belongs, because bipolar disorder is deeply sensitive to rhythm.
A holistic layer supports stability through:
- sleep protection (consistent schedule, bedtime routines, managing screen exposure)
- stress load management (reducing “always on” patterns that trigger episodes)
- nutrition and movement (not as a cure, but as brain-supporting habits)
- substance use screening (because substances can destabilize mood cycling)
- family and relationship alignment (so home becomes supportive, not reactive)
WHO also highlights how bipolar disorder affects many areas of life and is often linked to stigma and discrimination. Holistic approach addresses that reality too, helping you build a stable life, not just manage symptoms.
What Should Patients Expect During Integrated Therapy for Bipolar Disorder
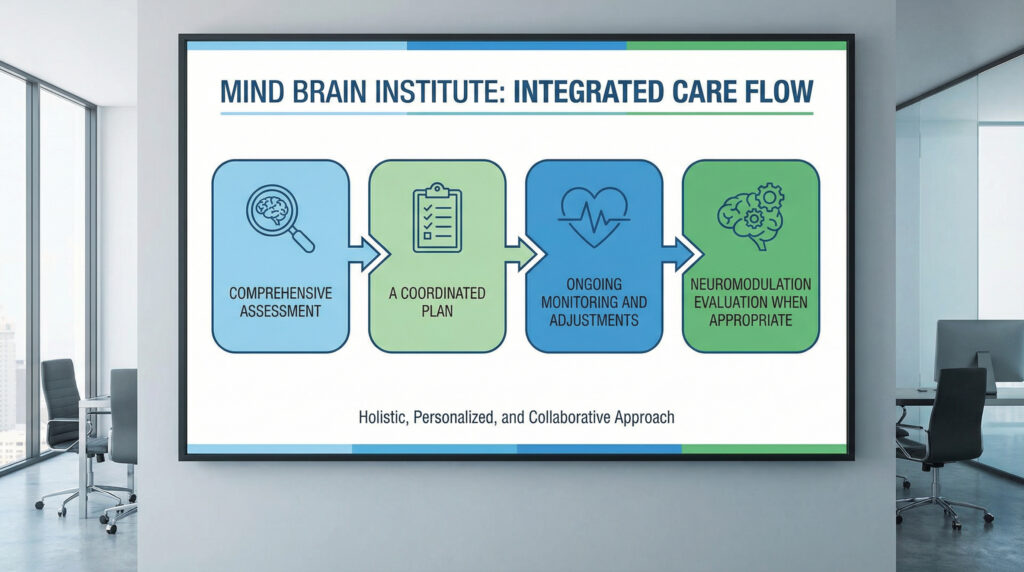
At Mind Brain Institute, integrated care typically follows a clear flow:
- Comprehensive assessment: We explore symptom history, episode patterns, sleep rhythm, family history, and treatment response.
- A coordinated plan: Medication and psychotherapy are aligned with shared goals (for example: stabilizing sleep first, then strengthening relapse prevention).
- Ongoing monitoring and adjustments: Bipolar treatment works best when it’s tracked. Small changes early can prevent big relapses later.
- Neuromodulation evaluation when appropriate: If depression remains stubborn, we discuss options like TMS, tVNS, neurofeedback and other relevant services, whether these fit your profile or not.
The result should feel like this: fewer surprises, more clarity, and a plan you can actually follow.
How Does Integrated Therapy Improve Quality of Life
The biggest win is not only fewer episodes. It’s the life that returns in between:
- improved relationships
- steadier work performance
- less fear of relapse
- better self-trust
- faster recovery when mood shifts happen
Integrated care helps you move from “surviving cycles” to building stability that holds—even when life gets stressful.
Overall…
Bipolar disorder is complex, but your treatment should not feel chaotic. When psychiatry, psychotherapy, and neuromodulation work together, stability becomes more achievable.
At Mind Brain Institute, we believe care should be coordinated, evidence based, and deeply personalized. Integrated therapy for bipolar disorder is not about doing more treatments. It is about doing the right treatments together, in the right order, with continuous guidance.
If you are ready to move from reactive crisis management to proactive stability, integrated care may be the step that changes everything.
Dr. Anuranjan Bist stands as a pioneering figure in the field of mental health, seamlessly blending traditional psychiatric methods with holistic wellness practices. With a profound understanding of the human mind and body, Dr. Bist has redefined therapeutic approaches by integrating Transcranial Magnetic Stimulation (TMS) and Ketamine therapy with ancient yoga techniques, showcasing his innovative spirit and dedication to comprehensive care.


