TMS for Postpartum Depression & Anxiety Is a Safe and Effective Treatment for New Mothers
You prepared for sleepless nights. You prepared for diaper changes. You prepared for your life to look different.
What many mothers are not prepared for is the quiet emotional shift that can follow childbirth, the heaviness, the racing thoughts, the unexplained tears, or the unsettling sense of disconnection. Instead of joy, you may feel guilt for not feeling joyful enough.
According to research, about 1 in 8 women experience symptoms of postpartum depression. Whereas, globally, the World Health Organization estimates that 10–20% of mothers experience postpartum depression or anxiety.
The good news? Postpartum depression is treatable. And today, more mothers are exploring non-medication options like TMS for postpartum depression as a safe and evidence-based alternative.
Let’s walk through what you need to know.
What Is Postpartum Depression?
Postpartum depression is a clinically recognized mood disorder that can develop during pregnancy or within the first year after childbirth. It is not simply an emotional reaction to the stress of caring for a newborn. Instead, it reflects measurable changes in brain chemistry, hormonal regulation, and stress response systems. After delivery, levels of estrogen and progesterone drop sharply, influencing neurotransmitters such as serotonin and dopamine that help regulate mood. At the same time, sleep disruption, physical recovery, and psychological adjustment to motherhood place additional strain on the brain. For some women, these combined biological and environmental factors trigger a depressive episode. Postpartum depression is a medical condition, not a weakness, and it requires the same evidence-based attention and care as any other health disorder.
What Are the Symptoms of Postpartum Depression and Anxiety?
Postpartum depression often overlaps with postpartum anxiety. Many women experience both simultaneously. Common symptoms include:
Emotional symptoms
Emotional symptoms refer to noticeable changes in your mood and feelings that persist and feel difficult to control. In postpartum depression and anxiety, these emotions are intense, frequent, and interfere with daily life. Common emotional symptoms include:
- Constant worry about the baby’s health
- Irritability or anger
- Feeling disconnected
- Crying frequently
Physical symptoms
Physical symptoms are bodily changes that occur alongside emotional distress. In postpartum depression and anxiety, your body often reflects what your mind is struggling to process. Common physical symptoms include:
- Insomnia even when the baby sleeps
- Panic attacks
- Racing heart
- Brain fog
Cognitive symptoms
Cognitive symptoms affect how you think, process information, and interpret situations. In postpartum depression and anxiety, your thoughts may feel overwhelming, repetitive, or frightening. Common cognitive symptoms include:
- Intrusive thoughts
- Fear of harming the baby (which can be terrifying but does not mean you will act on them)
If these symptoms persist for more than two weeks, seeking postpartum depression help is important. Early intervention leads to better outcomes.
What Are the Standard Treatment Options for Postpartum Depression?
Standard postpartum depression treatment typically includes psychotherapy, medication, and supportive care. The first-line approach for many women is talk therapy, especially Cognitive Behavioral Therapy (CBT) or Interpersonal Therapy (IPT). These evidence-based therapies help mothers manage negative thought patterns, process emotional changes, and rebuild coping skills.
For moderate to severe cases, doctors may recommend antidepressant medication, particularly selective serotonin reuptake inhibitors (SSRIs). Many SSRIs are considered relatively safe during breastfeeding, though decisions should always be individualized with a healthcare provider.
In some situations, a newer FDA-approved medication specifically for postpartum depression may be prescribed.
Support groups, family involvement, proper sleep, and nutritional care also play an important role. The right treatment plan depends on symptom severity, medical history, and personal preference, which is why professional evaluation is essential.
What Is TMS Therapy and How Does It Work?
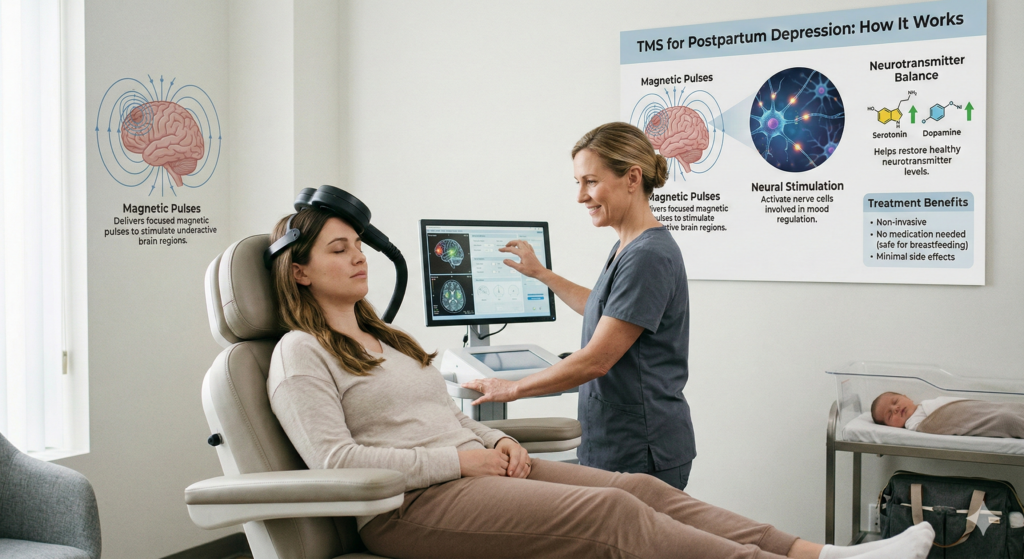
TMS stands for Transcranial Magnetic Stimulation. It is a non-invasive, FDA-approved treatment for major depressive disorder that uses magnetic pulses to stimulate specific areas of the brain associated with mood regulation. Here’s how it works:
- A magnetic coil is placed gently on your scalp.
- It delivers targeted magnetic pulses.
- These pulses stimulate underactive brain regions, particularly the prefrontal cortex.
Over time, neural pathways involved in mood improve. Unlike medication, TMS therapy does not circulate through your bloodstream. It does not affect your entire body. It directly targets brain circuits linked to depression.
According to the U.S. Food and Drug Administration (FDA), TMS is approved for treatment-resistant depression. This makes TMS for postpartum depression an increasingly promising option, especially for women seeking drug-free alternatives.
Why Is TMS for Postpartum Depression Considered a Safe Treatment Option?
Safety is the first concern for any new mother. One of the major advantages of TMS for postpartum depression is that it is:
- Non-invasive
- Drug-free
- Systemic side-effect free
- Safe during breastfeeding
Because TMS does not involve medication, there is no transfer through breast milk. That alone provides enormous peace of mind.
Common side effects are typically mild and may include:
- Scalp discomfort
- Mild headache
- Temporary lightheadedness
- Severe side effects are rare.
For mothers looking for a safe depression treatment while breastfeeding, TMS for postpartum depression provides reassurance without compromising effectiveness.
Can TMS for Postpartum Depression Also Help With Anxiety Symptoms?
Yes, and this is important. Depression and anxiety share overlapping brain circuits. Research suggests that TMS may positively influence both mood and anxiety regulation. Many patients receiving TMS for postpartum depression report improvements in:
- Panic symptoms
- Constant worry
- Racing thoughts
- Emotional reactivity
Clinical studies indicate that TMS therapy for depression can also reduce comorbid anxiety symptoms. Since postpartum anxiety treatment often requires medication, having a non-medication alternative is a breakthrough.
For mothers experiencing both sadness and intense anxiety, TMS for postpartum depression may address both simultaneously.
Who Is a Good Candidate for TMS for Postpartum Depression?
You may consider TMS for postpartum depression if:
- Medication has not worked for you
- You want to avoid antidepressants
- You are breastfeeding and concerned about medication exposure
- You experience moderate to severe symptoms
- You prefer a non-medication treatment approach
However, evaluation by a qualified mental health professional is essential. At Mind Brain Institute, we conduct a comprehensive assessment before recommending TMS therapy for depression or postpartum anxiety treatment. This ensures safety, personalization, and better outcomes.
Is TMS Safe While Breastfeeding?
This question deserves clear reassurance. One reason many women consider TMS for postpartum depression is its safety during breastfeeding. Because the treatment does not involve medication and does not introduce chemicals into the bloodstream, there is no known transfer into breast milk. This significantly reduces concerns about infant exposure.
Clinical research and established treatment guidelines indicate that TMS is generally considered safe during lactation when administered under proper medical supervision. Reported side effects are typically mild and localized, such as temporary scalp discomfort.
That said, every mother’s situation is unique. It is important to consult your healthcare provider to determine whether TMS for postpartum depression is appropriate for you.
When Should a New Mother Seek Professional Help?
Every new mother feels overwhelmed at times. But if sadness, anxiety, or emotional numbness lasts longer than two weeks, it may be more than temporary adjustment. You should seek professional help if you experience persistent low mood, severe anxiety, panic attacks, difficulty bonding with your baby, or inability to manage daily tasks.
Immediate support is essential if you have thoughts of harming yourself or your baby. These thoughts can feel frightening, but they are a medical signal, not a moral failure.
Early intervention leads to better recovery outcomes. Speaking with your OB-GYN, primary care doctor, or a licensed mental health professional can help you access appropriate postpartum depression treatment and support. You do not have to wait until symptoms become unbearable. Seeking help early is a strong and responsible step toward healing.
Overall…
Motherhood is transformative, but it should not feel like constant emotional survival.
If you are struggling, it is not a personal failure. It is a medical condition. And medical conditions deserve proper treatment.
For women seeking a drug-free, evidence-based, and safe option, TMS for postpartum depression offers real hope. It targets the brain circuits responsible for mood without affecting your body systemically. Many mothers who felt stuck, exhausted, and disconnected have regained emotional balance through TMS for postpartum depression.
If you want to learn more about whether TMS for postpartum depression is right for you, schedule a professional consultation and explore your options.
Dr. Anuranjan Bist stands as a pioneering figure in the field of mental health, seamlessly blending traditional psychiatric methods with holistic wellness practices. With a profound understanding of the human mind and body, Dr. Bist has redefined therapeutic approaches by integrating Transcranial Magnetic Stimulation (TMS) and Ketamine therapy with ancient yoga techniques, showcasing his innovative spirit and dedication to comprehensive care.


