Sarah had tried everything for her treatment-resistant depression, including medications, therapy, and lifestyle changes. Nothing seemed to work. Then her psychiatrist mentioned TMS therapy, but with a difference: a clinic using advanced magnetic field optimization in TMS. Three months later, she describes the experience as “getting my life back.” What made the difference wasn’t just the treatment itself, but how precisely it was delivered.
The world of transcranial magnetic stimulation is undergoing a quiet revolution. While TMS has been around for decades, recent advances in coil technology and neuronavigation are transforming it from a somewhat imprecise intervention into a finely-tuned therapeutic tool. Let’s explore how magnetic field optimization in TMS is reshaping the landscape of brain stimulation therapy.
What Is Magnetic Field Optimization in TMS and Why Does It Matter?
Think of magnetic field optimization in TMS as the difference between a spotlight and a floodlight. Traditional approaches often used broader, less focused magnetic fields that stimulated larger brain areas. Modern optimization techniques allow clinicians to target specific neural circuits with remarkable precision.
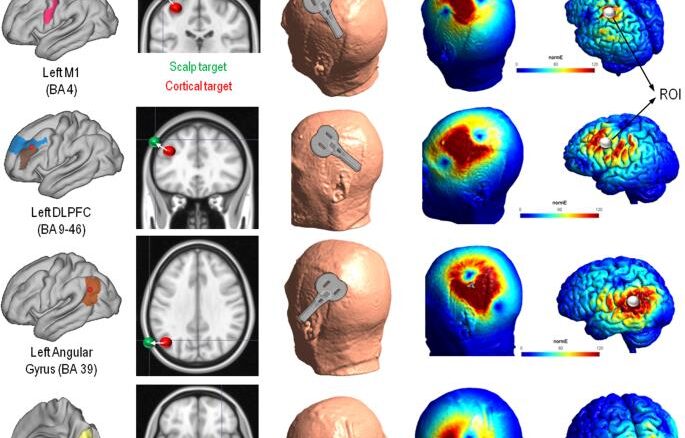
Here’s why this matters: the brain isn’t a uniform organ. Different regions control different functions, and the exact location of these regions varies slightly from person to person. When you’re trying to treat depression by stimulating the dorsolateral prefrontal cortex (DLPFC), being off by even a few millimeters can mean the difference between meaningful improvement and minimal response.
Magnetic field optimization in TMS involves fine-tuning three critical parameters: field strength, focality, and penetration depth. Too weak, and you won’t activate enough neurons. Too strong or too broad, and you risk stimulating areas you didn’t intend to target. This precision medicine approach recognizes that what works for one patient might need adjustment for another based on their unique brain anatomy and condition severity.
How Has Coil Technology Advanced in Recent Years?
The evolution of TMS coil technology reads like a story of increasing sophistication. Early figure-8 coils were revolutionary but had limitations; they could only reach superficial brain regions and had relatively broad stimulation patterns.
Enter the H-coil and Deep TMS technology. These innovations fundamentally changed what was possible with repetitive transcranial magnetic stimulation (rTMS). The H-coil’s unique design allows magnetic fields to penetrate more deeply into the brain, reaching areas such as the anterior cingulate cortex that traditional coils couldn’t effectively access. Research has shown that this deeper penetration opens new possibilities for treating conditions like OCD and certain depression subtypes that don’t respond to conventional TMS.
But depth isn’t the only frontier. Modern TMS coil technology has also embraced miniaturization and flexibility. Newer designs conform better to individual head shapes, ensuring more consistent magnetic field delivery session after session. Some systems now use multiple smaller coils that can be activated in specific sequences, creating more complex and targeted stimulation patterns.
These advances directly support magnetic field optimization in TMS by giving clinicians more tools to customize treatment. It’s no longer just about whether to use TMS, but which coil configuration, intensity, and pattern will work best for each patient’s specific condition and brain anatomy.
What Role Does Neuronavigation Play in Treatment Precision?
If advanced coils are the “what” of modern TMS, neuronavigation systems are the “where.” Imagine trying to hit a target the size of a grape while blindfolded—that’s essentially what early TMS practitioners faced. Neuronavigation changed everything.
These sophisticated systems use MRI scans of a patient’s brain to create a detailed 3D map. During treatment, real-time tracking ensures the coil stays positioned over the exact target area, accounting for small head movements and ensuring consistency across sessions. Some systems even use EEG-based navigation for functional targeting, identifying not just anatomical landmarks but areas of abnormal brain activity.
The impact on magnetic field optimization in TMS cannot be overstated. Studies from leading institutions demonstrate that neuronavigation significantly improves treatment outcomes by ensuring millimeter-level accuracy. When you’re targeting a specific neural circuit, that precision translates directly to better response rates and fewer sessions needed to achieve results.
Neuronavigation also helps clinicians understand why some patients respond better than others. By tracking exactly where stimulation was delivered and correlating that with outcomes, researchers are building increasingly sophisticated models of which brain areas to target for different conditions.
How Do Modern Systems Combine Coil Technology and Neuronavigation?
The real magic happens when advanced coils meet precision navigation. Today’s cutting-edge systems don’t just use these technologies in parallel—they integrate them into a seamless treatment platform.
Modern magnetic field optimization in TMS platforms incorporates AI and machine learning algorithms that analyze individual brain anatomy and suggest optimal coil positioning and stimulation parameters. Some systems can even adjust treatment in real-time based on monitoring of brain activity, creating a feedback loop that maximizes therapeutic benefit while minimizing side effects.
This integration enables personalized TMS therapy at a level that was unimaginable a decade ago. Clinicians can now map out treatment protocols that account for cortical thickness, gray matter density, and individual variations in brain structure. The system might recommend higher intensity for one patient and longer pulse trains for another, all optimized to deliver the right magnetic field strength to the right location.
This technological synergy is also driving our understanding of TMS-induced neuroplasticity. By combining precise stimulation with advanced brain imaging, researchers are uncovering exactly how magnetic fields trigger the neural changes that lead to symptom improvement.
What Are the Current Challenges in Magnetic Field Optimization?
Despite remarkable progress, magnetic field optimization in TMS still faces hurdles. The most obvious is cost; advanced neuronavigation systems and newer coil technologies require significant investment, which not all clinics can afford. This creates disparities in access to the most effective TMS treatment protocols.
Training represents another challenge. Operating these sophisticated systems requires expertise beyond basic TMS certification. Clinicians need to understand neuroanatomy, brain imaging, and the nuances of different stimulation parameters. There’s a learning curve that can slow adoption.
Standardization also remains elusive. While some centers achieve remarkable results with optimized protocols, others still use older approaches. The field lacks universal guidelines on exactly how to optimize treatment for different conditions and patient populations.
Perhaps most challenging is individual variability. Even with perfect technology, some patients respond better than others, and we don’t fully understand why. Ongoing research into biomarkers and predictive factors aims to address this, but it’s still a work in progress.
What Does the Future Hold for TMS Technology?
The trajectory is clear: magnetic field optimization in TMS will only get more sophisticated. Closed-loop systems that monitor brain activity and adjust stimulation in real-time are moving from research labs into clinical practice. Imagine a system that detects when your brain is in an optimal state for neuroplasticity and delivers pulses precisely at those moments; that’s not science fiction anymore.
Multi-site stimulation protocols are another frontier. Instead of targeting one brain area, future systems might simultaneously stimulate multiple connected regions, potentially producing faster and more robust improvements. Early results are promising.
Portability is also improving. While hospital-based systems will remain the gold standard for complex cases, smaller devices for maintenance therapy or home use are under development. This could make long-term management of chronic conditions more feasible and affordable.
How Can Patients Benefit from These Advancements Today?
If you’re considering TMS therapy, ask potential providers about their approach to magnetic field optimization in TMS. Clinics using neuronavigation and advanced coil technology generally achieve better outcomes. Questions to ask include: Do they use MRI-guided navigation? What type of coil system do they employ? How do they customize treatment protocols?
Don’t be swayed by marketing alone; look for providers who can explain their technical approach in understandable terms and who stay current with emerging research. The best clinics view each patient as unique and adjust their protocols accordingly.
The evolution of magnetic field optimization in TMS represents one of psychiatry’s most exciting frontiers. By marrying sophisticated coil technology with precision neuronavigation, we’re transforming a promising treatment into an increasingly reliable one. For patients like Sarah who’ve struggled with treatment-resistant conditions, these advances represent something precious: genuine hope backed by genuine science.
The future of brain stimulation therapy isn’t just about doing TMS; it’s about doing it with unprecedented precision, personalization, and effectiveness. That future is already arriving, one optimized magnetic pulse at a time.
Dr. Anuranjan Bist stands as a pioneering figure in the field of mental health, seamlessly blending traditional psychiatric methods with holistic wellness practices. With a profound understanding of the human mind and body, Dr. Bist has redefined therapeutic approaches by integrating Transcranial Magnetic Stimulation (TMS) and Ketamine therapy with ancient yoga techniques, showcasing his innovative spirit and dedication to comprehensive care.