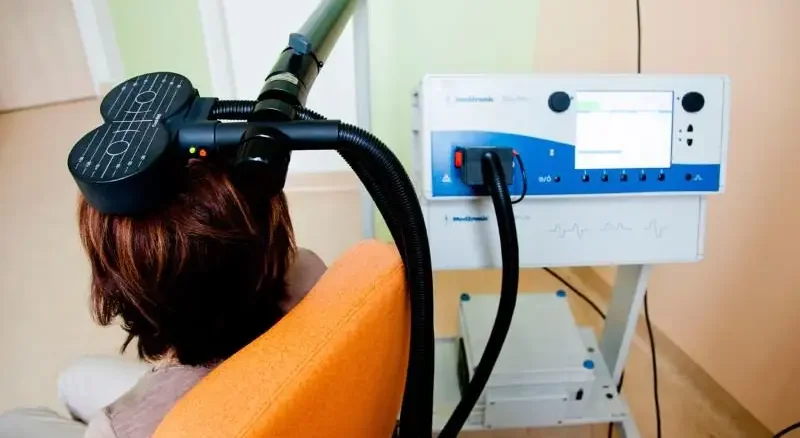
TMS-The Future of TMS: Innovations and Emerging Uses
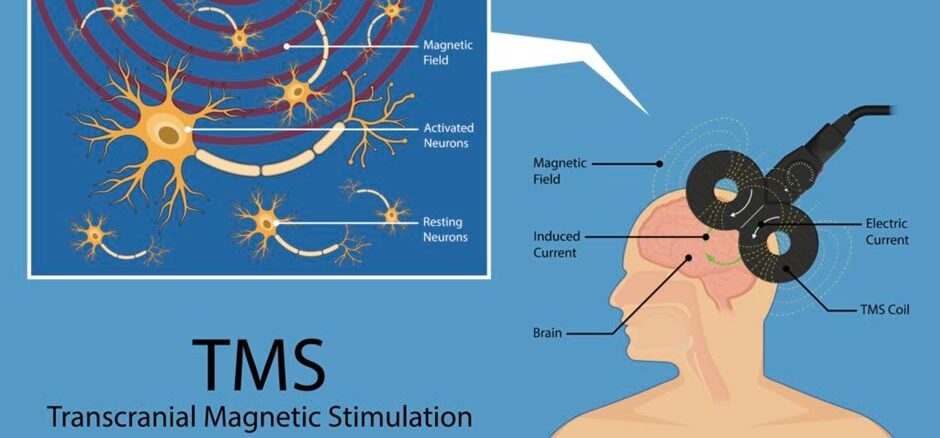
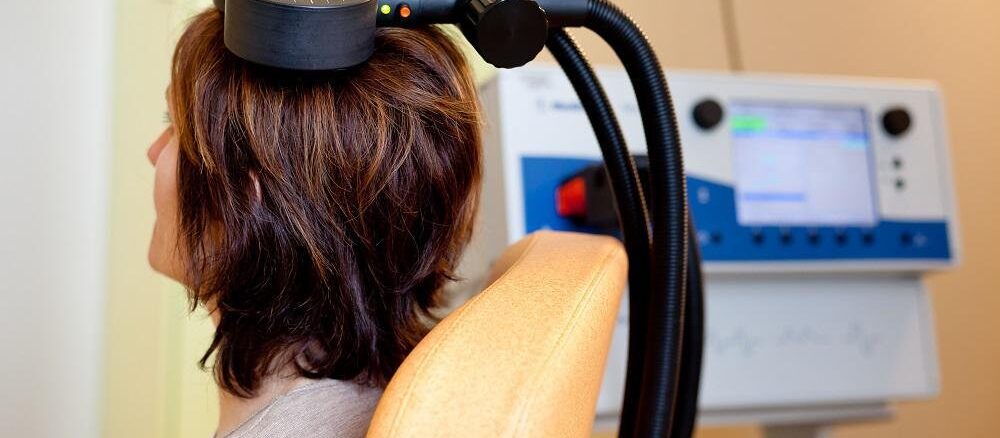
Transcranial Magnetic Stimulation (TMS) has been a beacon of hope for many suffering from depression and other neurological disorders. As we venture into the future, TMS is poised for a revolutionary leap forward, with advancements in technology and expanding applications that promise to transform the landscape of psychiatric and neurological treatment. This blog post delves into the horizon of TMS therapy, exploring the innovative technologies, new therapeutic targets, and burgeoning applications that are set to redefine its role in medicine. Technological Advancements in TMS The core of TMS’s evolution lies in technological refinement. Future devices are expected to offer unprecedented precision in targeting brain regions, thereby enhancing efficacy and minimizing side effects. Real-time brain imaging and mapping technologies, such as fMRI (functional Magnetic Resonance Imaging) or PET (Positron Emission Tomography), are being integrated with TMS to provide live feedback, enabling clinicians to tailor treatments to the individual’s neuroanatomy in real-time. Moreover, the development of portable TMS devices could democratize treatment, making it accessible to a broader population. These devices, potentially wearable, would allow for continuous or on-demand treatment, opening up possibilities for managing chronic conditions outside the clinical setting. Enhanced Protocols and Personalization The future of TMS lies not only in hardware but also in the sophistication of treatment protocols. Adaptive algorithms, powered by artificial intelligence (AI), are being designed to personalize treatment in real-time, adjusting parameters like intensity, frequency, and duration to optimize outcomes. This individualized approach could significantly improve response rates, particularly in treatment-resistant cases. New Therapeutic Targets Beyond depression, the scope of TMS is expanding to include a wide array of neurological and psychiatric conditions. Research is underway to explore its efficacy in treating Alzheimer’s disease, epilepsy, Parkinson’s disease, and stroke rehabilitation, among others. The principle underlying these applications is neuroplasticity—the brain’s ability to reorganize itself. By selectively stimulating or inhibiting specific brain regions, TMS may facilitate the reestablishment of normal neural pathways or help in creating new ones, offering hope for conditions previously deemed untreatable. TMS in Cognitive Enhancement Another intriguing frontier for TMS is cognitive enhancement in healthy individuals. Studies are investigating its potential to improve memory, attention, and other cognitive functions. This raises ethical questions about the use of TMS for non-therapeutic purposes, such as enhancing learning or performance in healthy individuals, but also opens up exciting possibilities for understanding and augmenting human cognition. Expanding Applications for Other Conditions The applicability of TMS is being explored beyond the brain, in conditions such as fibromyalgia and chronic pain, where altered neural activity is a contributing factor. The anti-inflammatory effects of TMS, though not fully understood, offer another avenue for treating a variety of inflammatory conditions, potentially including autoimmune diseases. Conclusion The future of TMS therapy is bright, with groundbreaking advancements on the horizon that promise to expand its therapeutic reach, enhance its efficacy, and revolutionize the treatment of neurological and psychiatric conditions. As technology advances and our understanding of the brain deepens, TMS stands as a testament to the potential of innovation to reshape medicine. The journey ahead is fraught with challenges, but the possibilities are as vast as the human mind itself.