Depression is not rare, and it is not simple. The World Health Organization estimates that about 5% of adults globally live with depression, and many do not get enough relief from standard treatment alone. That matters because for a meaningful group of patients, the problem is not just low mood. It is a deeper pattern of stuck brain circuits, poor emotional flexibility, and symptoms that keep returning despite medication, therapy, or both.
This is where newer brain-based treatments have started to attract serious attention. One of the most interesting ideas in modern psychiatry is Combination therapy with TMS and Psychedelics. In simple terms, it asks a smart clinical question: what if one treatment could make the brain more open to change, while the other could guide that change in a more targeted direction? That is the scientific logic behind what some researchers now describe as Psychedelic-assisted TMS therapy.
At the moment, this is still an emerging area, not a routine standard of care. But it is not science fiction either. Early evidence, especially around TMS combined with ketamine-based treatment, suggests this approach may offer meaningful benefits for some people with treatment-resistant depression.
What Is Combination Therapy with TMS and Psychedelics?
Combination therapy with TMS and Psychedelics refers to the use of transcranial magnetic stimulation, or TMS, alongside a psychedelic or psychedelic-like intervention in an effort to improve outcomes in mood disorders, especially depression. TMS is a noninvasive brain stimulation treatment that uses magnetic fields to influence activity in specific brain networks involved in mood regulation. Brain stimulation therapies are already recognized by the NIMH as important tools in mental health treatment, especially when other options have not worked well enough.
The psychedelic side of this equation needs careful explanation. In real-world clinical settings today, the best-known example is not necessarily psilocybin or MDMA, but ketamine or esketamine. Strictly speaking, ketamine is not a classic psychedelic in the same category as psilocybin. But in psychiatric practice, it is often discussed in the same broader conversation because it can rapidly alter perception, emotional processing, and neuroplasticity in supervised settings. That is why much of today’s practical discussion around Psychedelic-assisted TMS therapy centers on TMS plus ketamine-based care.
How Does the Brain Respond to This Combination Therapy?
To understand why this approach is exciting, it helps to think of depression as more than a “chemical imbalance.” Depression also involves disrupted brain networks. Some circuits become underactive, some become overly rigid, and some stop communicating in healthy ways. TMS is appealing because it can noninvasively stimulate targeted regions of the brain linked to mood, cognition, and motivation.
Psychedelic treatments, especially psilocybin and ketamine-related approaches, are interesting for a different reason. Research suggests they may temporarily loosen rigid patterns in the brain, including changes in the default mode network, a system associated with self-referential thinking and rumination. That matters because many depressed patients do not just feel sad; they feel mentally trapped in the same painful loops. When the brain becomes more flexible, therapy and other interventions may be more effective.
That is the central promise of Combination therapy with TMS and Psychedelics: one treatment may increase openness to change, while the other may help direct and reinforce healthier brain activity. It is a neuroplasticity story. Not magic, not hype, but a real scientific attempt to help the brain relearn.
What Conditions Might Benefit from This Approach?
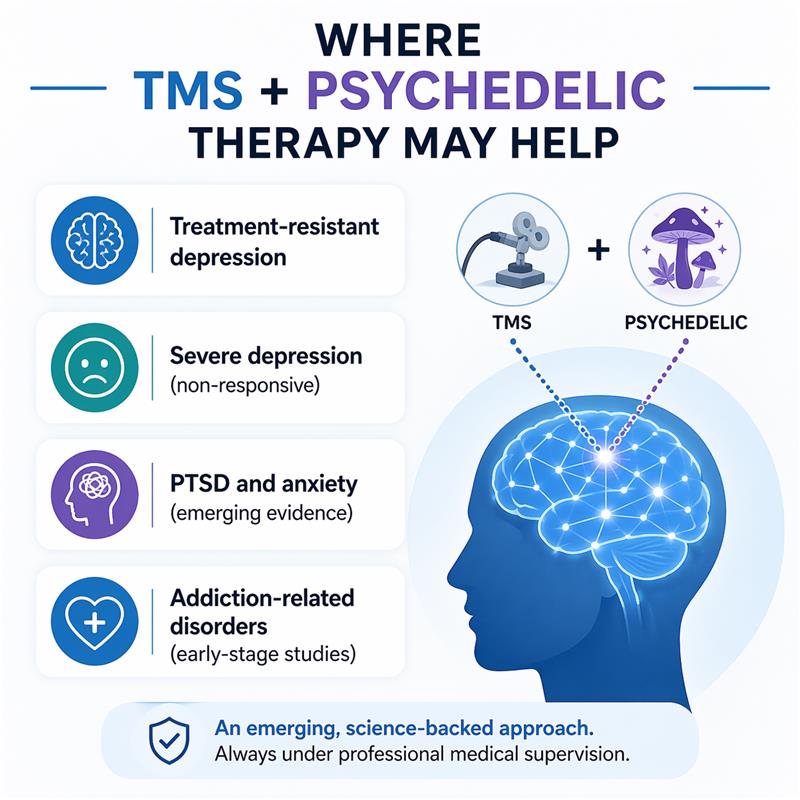
The clearest target is treatment-resistant depression. If someone has tried appropriate medication, psychotherapy, or both without enough improvement, Combination therapy with TMS and Psychedelics becomes a meaningful research question and, in some cases, a clinical consideration when ketamine is involved.
There is also growing interest in related conditions such as PTSD, anxiety disorders, and addiction, but the evidence is not equally strong across all diagnoses. That distinction matters. Good psychiatric writing should never blur “promising” into “proven.” Right now, depression, especially treatment-resistant depression, remains the most grounded area of interest.
Is Combination Therapy with TMS and Psychedelics Safe?
Safety depends on what exactly is being combined, who is being treated, and how carefully the treatment is supervised. TMS itself is generally considered safe when delivered by trained professionals. Psychedelic-based interventions require far more screening and structure because they can affect perception, blood pressure, dissociation, anxiety, and emotional intensity.
That is why Psychedelic-assisted TMS therapy should never be discussed as a DIY wellness trend. It belongs in a medical framework with psychiatric evaluation, informed consent, monitoring, and a clear follow-up plan. The future of this field will depend not only on whether it works, but on whether it is delivered responsibly.
What Does Current Research Actually Say?
The honest answer is this: the signal is promising, but the evidence base is still early. For TMS plus ketamine, the literature is encouraging enough to deserve attention. For TMS plus classic psychedelics such as psilocybin, the field is more experimental, though active trials are underway.
On the psychedelic side more broadly, recent reviews and meta-analyses suggest psilocybin-assisted therapy may reduce depressive symptoms and may do so with meaningful effect sizes in selected settings. But that is not the same as saying we already know the best protocol, the ideal patient profile, or the long-term risk-benefit balance of combining it with TMS.
That distinction is important for trust. Science is moving forward. It is not finished.
What Does This Mean for the Future of Depression Treatment?
The future of depression care is likely to be more personalized, more circuit-based, and less dependent on the old one-size-fits-all model. That is why Combination therapy with TMS and Psychedelics matters. It reflects a broader shift in psychiatry: away from simply suppressing symptoms and toward actively helping the brain become more adaptable, more responsive, and more recoverable.
For patients, that future should bring hope, but also clarity. Not every new treatment is ready for everyone. Not every promising headline becomes good medicine. The right next step is always careful evaluation, not blind enthusiasm.
If you are exploring advanced options for depression, this is a good place to connect the conversation back to fundamentals: a proper diagnosis, an evidence-based treatment plan, and care that looks at both symptoms and brain function.
At Mind Brain Institute, we focus on evidence-based, brain-centered treatments that combine modern neuroscience with personalized care to help individuals move beyond treatment-resistant conditions.
Dr. Anuranjan Bist stands as a pioneering figure in the field of mental health, seamlessly blending traditional psychiatric methods with holistic wellness practices. With a profound understanding of the human mind and body, Dr. Bist has redefined therapeutic approaches by integrating Transcranial Magnetic Stimulation (TMS) and Ketamine therapy with ancient yoga techniques, showcasing his innovative spirit and dedication to comprehensive care.